Female Genital Mutilation (FGM) Practice Guidance
Joint City of York Safeguarding Children’s Partnership and North Yorkshire Safeguarding Children’s Partnership
Aim and Purpose
This guidance should be considered in conjunction with other relevant safeguarding guidance, including but not limited to, Multi-agency Statutory Guidance on Female Genital Mutilation (updated 2018), Working Together to Safeguard Children, and additional local procedures and practice guidance available at North Yorkshire Safeguarding Children Partnership (NYSCP) and City of York Safeguarding Children Partnership (CYSCP). This guidance is not intended to replace wider safeguarding guidance, but to provide additional advice on Female Genital Mutilation (FGM).
Definitions
For the purpose of this guidance, the following definitions apply:
Adult/Woman: ‘Adult’ is defined as a person aged 18 years or over.
Child / Young Person: As defined in the Children Acts 1989 and 2004, ‘child’ means a person under the age of 18. This includes young people aged 16 and 17 who are living independently; their status and entitlement to services and protection under the Children Act 1989 is not altered by the fact that they are living independently.
Key points:
FGM is illegal in England and Wales under the Female Genital Mutilation Act 2003[3].
As amended by the Serious Crime Act 2015, the Female Genital Mutilation Act 2003 now includes:
- An offence of failing to protect a girl from the risk of FGM,
- Extra-territorial jurisdiction over offences of FGM committed by abroad by UK nationals and those habitually (as well as permanently) resident in the UK,
- Lifelong anonymity for victims of FGM,
- FGM Protection Orders (FGMPOs) which can be used to protect girls and women at risk (see FGMPO Factsheet), and
- A mandatory reporting duty which requires specified professionals to report known cases of FGM in under 18s to the police.
In England and Wales, criminal and civil legislation on FGM is contained in the Female Genital Mutilation Act 2003
What is Female Genital Mutilation?
The World Health Organisation defines FGM as “…all procedures that involve partial or total removal of the external female genitalia, or other injury to the female genital organs for non-medical reasons”.
The Female Genital Mutilation Act 2003 (as amended) narrows the definition of FGM to not include:
- a surgical operation on a girl that was necessary for her physical or mental health, or
- a surgical operation on a girl who was in any stage of labour, or had just given birth, for purposes connected with the labour or birth
It is frequently a very traumatic and violent act of the victim and can cause harm in many ways. The practice can cause severe pain and there may be immediate and / or long-term health consequences, including mental health problems, difficulties in childbirth, causing danger to the child and mother; and / or death.
The age at which FGM is carried out varies enormously according to the community. The procedure may be carried out shortly after birth, during childhood or adolescence, just before marriage or during a woman’s first pregnancy.
FGM is a criminal offence – it is child abuse and a form of violence against those subjected to it, and therefore should be treated as such. Cases should be dealt with as part of existing North Yorkshire structures, policies and procedures on child protection (see, “Worried about a child?” and NYSCP Procedures) and the “Joint Multi-Agency Safeguarding Adults Policy and Procedures” for safeguarding adults. There are, however, particular characteristics of FGM that front-line professionals should be aware of to ensure that they can provide appropriate protection and support to those affected.
Legislation and Policy
The Female Genital Mutilation Act 2003 (with amendments from the Serious Crime Act 2015) makes it a criminal offence to:
- Excise, infibulate or otherwise mutilate the whole or any part of a female’s labia majora, labia minora or clitoris (subject to limited exemptions for mental or physical health)
- Aid, abet, counsel or procure a female to excise, infibulate or otherwise mutilate the whole or any part of her own labia majora, labia minora or clitoris, or
- Aid, abet, counsel or procure a person who is not a United Kingdom national or permanent United Kingdom resident to do a relevant act of female genital mutilation outside the United Kingdom
- This Act has extra-territorial extensions, i.e. if a person commits any of the above offences in another country it would be treated as if the offence had occurred in the United Kingdom. A person convicted of an offence under the FGM Act 2003 is liable to imprisonment between six months and fourteen years.
If a female genital mutilation offence is committed against a child under the age of 16, each person who is responsible for the child at the time FGM took place is also guilty of an offence. A person is ‘responsible’ for a child if they have parental responsibility for and frequent contact with the child or the person is over 18 years of age and has assumed (and not relinquished) responsibility for caring for the child in the manner of a parent.
What are the types of FGM?
| Type | Description | |
| 1 | Clitoridectomy | Partial or total removal of the clitoris (a small, sensitive and erectile part of the female genitals) and, in very rare cases, only the prepuce (the fold of skin surrounding the clitoris). |
| 2 | Excision | Partial or total removal of the clitoris and the labia minora, with or without excision of the labia majora (the labia are “the lips” that surround the vagina). |
| 3 | Infibulation | Narrowing of the vaginal opening through the creation of a covering seal. The seal is formed by cutting and repositioning the inner, or outer, labia, with or without removal of the clitoris. |
| 4 | Other | All other harmful procedures to the female genitalia for non-medical purposes, e.g. pricking, piercing, incising, scraping and cauterizing the genital area. |
Identifying a person at risk of FGM
Where a person is thought to be at immediate risk of FGM taking place or about to take place, practitioners must be alert to the need to act quickly before the person undergoes FGM either in the UK or abroad.
Indications that FGM may be about to take place:
- The family comes from a community that is known to practice FGM (it may also be possible that they will practice FGM if a female family elder is around);
- Parents requesting permission for their child to be taken out of school two weeks before or after the summer holidays (recovery period can be up to 8-10 weeks);
- A person talking about a long holiday to her country of origin or another country where the practice is prevalent
- A child talking about ‘becoming a woman’ or ‘rites of passage’
- A child talking about new clothing or special outfits
- A child may confide in a professional that they are about to undergo a “special procedure” or attend a special occasion
- Becoming withdrawn or acting out of character
- There are older females in the family (e.g. older sister/s, mother) who have undergone FGM
- Any female child born to a woman who has been subjected to FGM must be considered to be at risk, as must other female children in the extended family
- Any female who has a sister who has already undergone FGM must be considered to be at risk, as must other females in the extended family
- A relative or ‘cutter’ visiting from territories known to practice FGM
- Running away or planning to run away from home.
Identifying a person who has been subject to FGM
Indications that FGM may have already taken place:
- A child may spend long periods of time away from the classroom during the day with urinary or menstrual problems if they have undergone Type 3 FGM. Frequently, females who have undergone FGM find it harder to urinate, and it will therefore take longer to pass urine
- There may be prolonged absences from school with noticeable behaviour changes on the child’s return
- A child requiring to be excused from physical exercise lessons without the support of their GP and very often using the excuse that females of her faith can’t exercise
- A child may confide in a professional or ask for help
- Asking for help, and or needing extra support but not being explicit about what the problem is
- Difficulty walking, sitting or standing.
- Reluctance to have routine medical examinations.
Professionals encountering a person who has undergone FGM should be alert to the risk of FGM in relation to:
- Younger siblings;
- Daughters they may have in the future;
- Extended family members.
Responding to a child / young person who is at risk or who has been subject to FGM
The appropriate response to FGM, whether at risk or who has been subject to the procedure, is to follow safeguarding procedures to ensure:
- Immediate protection and support for the child / young person; and
- That the practice is not repeated with other members of the family, household or community, including any unborn children.
In addition, an appropriate response to a person who is at risk of FGM can include:
- Seeing the person on their own and creating an opportunity for them to disclose further information
- Using simple language and straightforward questions
- Using terminology that the person will understand, e.g. the person may not view the procedure as an illegal practice
- Being sensitive to the fact that the person may be loyal to those who subjected them to the procedure
- Arranging for an interpreter if this is necessary and appropriate (interpreters must be made aware of the subject they will be covering and that they are comfortable with this) – for further information regarding interpreters, please contact the Customer Resolution Centre on 0300 131 2 131, or City of York Council Interpreting and Translation Service
- Allowing the person time to talk
- Getting accurate information about the urgency of the situation, if the person is at risk of being subjected to the procedure
- Informing the person how to contact you again
An appropriate response by professionals who encounter a person who has undergone the procedure of FGM includes:
- Being sensitive to the intimate nature of the subject
- Making no assumptions
- Asking straightforward questions
- Being ready to listen
- Being non-judgmental (condemning the illegal practice, but not blaming the person)
- Understanding how they may feel in terms of language barriers, cultural differences, and that they, their partner, and their family may feel they are being judged
- Being able to explain that FGM is illegal and that discussing this with you can be used to help protect them and prevent the illegal practice of FGM from taking place in the future.
- Arranging for a professional interpreter (interpreters must be made aware of the subject they will be covering and that they are comfortable with this).
General advice when approaching those who may have undergone FGM or are at risk of FGM
Other useful advice when speaking to a person who may have undergone FGM or parents of a child you believe could be at risk includes:
- Using appropriate terms
- Approach the subject sensitively
- Where an interpreter is needed, a female interpreter is essential – a family or community member must not be used to translate
- Be aware that reinfibulation (after childbirth) is also illegal.
Responding suitably is key, so that the appropriate immediate protection and support can be provided. Furthermore, responding appropriately will disseminate a message in communities that the illegal practice of FGM is taken seriously and agencies are responding to FGM in a sensitive and robust way.
FGM and Unborn Babies
Where FGM is identified in pregnancy, an honest and open conversation should take place between the practitioner, the pregnant woman and her partner. Professionals should seek support from their organisation’s translation services as required, and not rely on relatives or friends to interpret conversations. The practitioner should share the opposing statement, which can be obtained in the woman’s first language.(Statement opposing female genital mutilation – GOV.UK (www.gov.uk).
The practitioner must complete the government FGM risk assessment form with the pregnant woman. This will help inform any safeguarding referral that is required for the unborn baby or child/children within the household. FGM Professional Guidance Forms (publishing.service.gov.uk) Professionals should also follow the NYSCP/CYSCP Guidance on Unborn Babies.
Where the level of risk is deemed to be low, for example, where a woman/ young person is over the age of 16 has consensually had a genital piercing or tattoo, or parents are opposing FGM, not planning to travel, etc., then a referral to the local authority may not be required. However, vigilance for emerging concerns must be maintained by all professionals involved in her care. In type 4 genital piercing, health care professionals must be assured that any genital piercing or tattoo has been acquired without coercion.
Where FGM has been identified, under information sharing guidance, health care professionals must inform the parent/s of the need for information sharing with the GP and 0-19 service. FGM will then be highlighted on both the mother’s record and any female children in the family. Female Genital Mutilation Risk and Safeguarding (publishing.service.gov.uk)
Professionals have a duty to report to the police ‘known’ cases of FGM in under 18s which they identify in the course of their professional work. This may be either the pregnant woman herself who is under 18, or a pregnant woman who has a daughter/s under 18 who have undergone FGM. The practitioner should report to the police using the non-emergency 101 telephone number and make a referral to Children’s Social Care. Health partners will also need to complete an FGM Reporting Enhanced Dataset (see your local Trust guidance).
During pregnancy, if the unborn is known to be female, gender unknown, or if the practitioner has reasonable cause to suspect that the unborn baby, as a result of her mother being a victim of FGM or a family history of FGM, is likely to suffer significant harm after birth then a referral to the Local Authority in which the unborn will live, must be made. The use of the opposing statement and FGM risk assessment (as above) may inform this decision-making.
Practitioners must ensure families are notified of the need for information sharing. Female Genital Mutilation Information Sharing (FGM – IS) is a national IT system for healthcare professionals. This government-mandated system requires an alert to be added to any female infant’s medical record where there is a family history of FGM. This will alert professionals working with the family that there is a risk of FGM, and services can therefore work with the family accordingly. (Health care professionals must follow their Trust guidance)
Mandatory Reporting Duty for all Professionals who identify FGM
All professionals (i.e. a teacher, social worker or healthcare professional) who, in the course of their work, believe that an act of FGM appears to have been carried out on a person who is aged under 18 years must notify the police. This includes cases where:
- A child or young person has told a professional that an act of FGM (however described) has been carried out on them, or
- The professional has observed physical signs indicating female genital mutilation has been carried out, and the professional has no reason to believe that the act was part of:
- a surgical operation on a female which is necessary for her physical or mental health, or
- a surgical operation on a female who is in any stage of labour, or has just given birth, for purposes connected with the labour or birth
The professional who identifies FGM in a female under 18 years must call 101 to make a report. When making an FGM notification to the police the professional must have details of:
- Person’s name, date of birth and address
- Name and contact details of the professional
- Name and contact details of the local safeguarding lead – Midwifery or Adult Safeguarding Lead
It is best practice when making notifications to the police to ensure:
- The notification is made on the same working day as FGM was identified calling via 101 to make a report
- Local safeguarding lead within your organisation is updated within one day
- All decisions and actions taken are recorded
If you believe that the person is in immediate danger you must act immediately, which may include calling 999. Mandatory reporting is only one part of safeguarding against FGM. Always ask your safeguarding lead if in doubt.
If the woman is over 18 when she discloses/FGM is identified, the mandatory duty to report does not apply and you should follow follow either North Yorkshire or City of York local safeguarding adults procedures
In all cases, professionals should also consider whether there are other people within the household, extended family and community who may be at risk of or may have been subject to FGM and whether anyone should be referred to the Children and Families Service. If the professional identifies an adult at risk of, or having been subjected to FGM, either North Yorkshire or City of York local safeguarding adults procedures should be followed.
Below illustrates the local procedures to be followed if there is a child / young person identified who has undergone FGM or is at risk of FGM.
FGM Local Procedure
When a child or young person is identified who has undergone FGM or is at risk of FGM
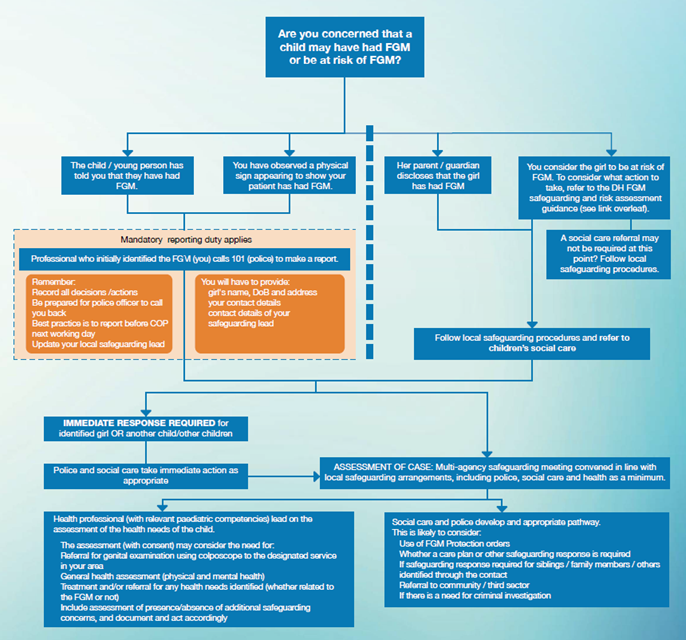
The Medical Response to North Yorkshire and York Children and Young People suspected of being subject to FGM
If FGM Is suspected in a child or young person normal safeguarding procedures should be followed.
If the strategy meeting decides a medical is needed to confirm if there are physical signs of FGM a referral should be made to the Department of Community Paediatrics at Leeds Community Health Care NHS Trust lcht.community.paediatrics4@nhs.net.
If the child has medical needs that need assessment and treatment, whether these are due to the FGM or another cause, these should be coordinated by the local paediatric service.
The purpose of an FGM medical is to establish if FGM has occurred, to support legal and safeguarding investigations and to ensure appropriate medical care. The medical examinations need to be of a high quality carried by a doctor with expertise in this area. To achieve this, the medicals need to be carried out in a planned way in a none urgent clinic. Following receipt of the referral for an FGM medical, the team will endeavour to see the child as soon as there is capacity and wherever possible, within one month of receipt of the referral.
Additional Guidance for NHS Staff
The Department for Health has produced additional guidance for NHS organisations so they can meet the requirements to collect and submit data about patients with FGM.
The guidance relates to the Female Genital Mutilation (FGM) Enhanced Dataset by the Health and Social Care Information Centre and the forthcoming professional duty about FGM to be published in September 2015. The following organisations are required to have regard to the FGM Enhanced dataset standard from September 2015:
- General Practice
- Mental Health Trusts
- Acute Trusts (mandatory since 1 July 2015)
Sexual health and GUM (Genito-Urinary Medicine) clinics, where patients do not have to provide their personal information, are out of scope, but these services are nonetheless reminded of their responsibilities to share information to ensure appropriate safeguarding responses are put in place every time this becomes necessary.
The flowchart below from the Department of Health outlines the FGM Safeguarding Pathway for NHS staff which includes mandatory reporting and reporting for the enhanced FGM dataset. The flowchart should be used by clinicians where a child or young person has made a disclosure of FGM or the clinician has observed a physical sign appearing to show the patient has been subject to FGM (this correlates to the left-hand side of the pathway on page 11) :
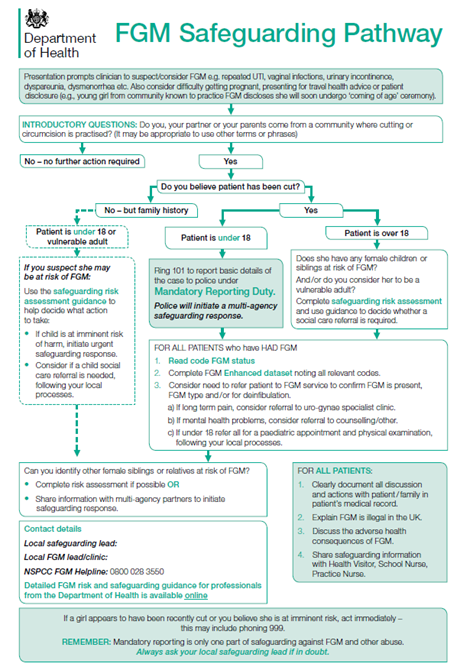
The data collected is sent to the Health and Social Care Information Centre (HSCIC), where it is anonymised, analysed and published in aggregate form. Personal information is only collected as part of the FGM Enhanced dataset for internal data quality assurance and to avoid duplicate counting. A woman or child’s personal details will never be published in the national aggregate reports and will never be passed to anyone outside HSCIC. This work specifically will not pass any personal details to the police or social services -the collection of this data will not trigger individual criminal investigations.
Further information can be accessed from:
Support Services
If you or the person you are concerned about is in danger and immediate action is required, you should ring the emergency services on 999.
If you have concerns about a person and you wish to speak to someone or make a referral, please use the following contacts:
North Yorkshire Council Customer Resolution Centre:
Open Monday to Friday 9.00am to 5.00pm
All areas: 0300 131 2 131
Emergency Duty Team (all other hours): 0300 131 2 131
For making a referral for a child under 18 years of age, please visit the NYSCP website at:
For making a referral for an adult 18 years or older, please visit the NYSAB website at:
City of York Council Multi-Agency Safeguarding Hub (MASH):
If you have a concern that a child is vulnerable or at risk of significant harm please contact the MASH Team:
Phone: 01904 551900
Email: MASH@york.gov.uk
Outside office hours, at weekends and on public holidays contact the emergency duty team telephone: 01609 780780
If you need to make a safeguarding referral to Children’s Social Care about a child or young person who has been or may be hurt or neglected or who has significant vulnerabilities please use the MASH Referral Form, which can be found on the CYSCP Concerned About A Child webpage
For making a referral for an adult 18 years or older, please visit the York Safeguarding Adults Board.
North Yorkshire Police
Call 101 to make a mandatory report of FGM to the police where a female under 18 years of age has disclosed or you have observed FGM has taken place. If a child is in immediate danger, call 999.
Appendix – Additional Guidance on FGM
Cultural Underpinnings
Female genital mutilation is underpinned by a mix of cultural and social factors within families and communities.
- Where FGM is a social convention, the social pressure to conform to what others do and have been doing is a strong motivation to perpetuate the practice
- FGM is often considered a necessary part of raising a child, and a way to prepare them for adulthood and marriage
- FGM is often motivated by beliefs about what is considered proper sexual behaviour, linking procedures to premarital virginity and marital fidelity. FGM in many communities is believed to reduce a woman’s libido and, therefore believed to help her resist “illicit” sexual acts. When a vaginal opening is covered or narrowed (Type 3 FGM), the fear of the pain of opening it, and the fear that this will be found out, is expected to further discourage “illicit” sexual intercourse among females with this type of FGM
- FGM is associated with cultural ideals of femininity and modesty, which include the notion that females are “clean” and “beautiful” after the removal of body parts that are considered “male” or “unclean”
- Though no religious scripts prescribe the practice, practitioners often believe the practice has religious support
- In most societies, FGM is considered a cultural tradition, which is often used as an argument for its continuation
- In some societies, the recent adoption of the practice is linked to copying the traditions of neighbouring groups. Sometimes it has started as part of a traditional revival movement
- In some societies, FGM is practised by new groups when they move into areas where the local population practices FGM
Piercings, Tattoos and Vaginal Modification
Vaginal modification, including piercings, tattoos and other modifications are increasingly common and can be a lifestyle choice by individuals. However, practitioners need to be aware that such modifications may also be classed as Type 4 Female Genital Mutilation. When considering whether a female is at risk of FGM, practitioners should consider whether she was able to consent to the procedure and if that consent was not forced or coerced. Practitioners should also consider the extent of the modification (if known). It should be noted that females under 18 years of age would not normally be able to consent to vaginal modification, including piercings and tattoos.
Names for FGM
FGM is referred to by many names, including female cutting and female circumcision (the latter being an expression which implies the practice is similar to male circumcision). The degree of cutting is far more extensive than male circumcision, and the procedure often impairs a woman’s sexual and reproductive functions and ability to pass urine normally.
Terms Used for FGM in Other Languages
| Country | Term used for FGM | Language |
| CHAD – the Ngama Sara subgroup | Bagne Gadja | |
| GAMBIA | Niaka Kuyungo Musolula Karoola | Mandinka Mandinka Mandinka |
| GUINEA-BISSAU | Fanadu di Mindjer | Kriolu |
| EGYPT | Thara Khitan Khifad | Arabic Arabic Arabic |
| ETHIOPIA | Absum Megrez | Harrari Amharic |
| ERITREA | Mekhnishab | Tigregna |
| IRAN | Xatna | Farsi |
| KENYA | Kutairi Kutairi was ichana | Swahili Swahili |
| NIGERIA | Ibi/Ugwu Didabe fun omobirin/ ila kiko fun omobirin | Igbo Yoruba |
| SIERRA LEONE | Sunna Bondo Bondo/sonde Bondo Bondo | Soussou Temenee Mendee Mandinka Limba |
| SOMALIA | Gudiniin Halalays Qodiin | Somali Somali Somali |
| SUDAN | Khifad Tahoor | Arabic Arabic |
| TURKEY | Kadin Sunneti | Turkish |
International Prevalence of FGM
FGM is a deeply rooted practice, widely carried out mainly among specific ethnic populations in Africa and parts of the Middle East and Asia. It serves as a complex form of social control of a woman’s sexual and reproductive rights. The exact number of children and adults alive today who have undergone FGM is unknown, UNICEF estimates that over 200 million children and women in 31 countries, across three continents, have undergone FGM, with more than half of those subjected living in Egypt, Ethiopia and Indonesia..
The heat map below shows some of the most prevalent areas of Africa where FGM is practised. More information can be obtained from Female Genital Mutilation (FGM) Statistics published by UNICEF.
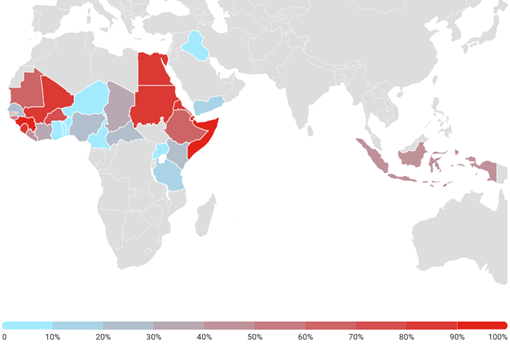
List of countries where female genital mutilation is prevalent
Benin
Burkina Faso
Cameroon
Central African Republic
Chad
Cote d’Ivoire (Ivory Coast)
Democratic Republic of Congo
Djibouti
Egypt
Eritrea
Ethiopia
Gambia
Ghana
Guinea
Guinea-Bissau
Kenya
Liberia
Mali
Mauritania
Niger
Nigeria
Senegal
Sierra Leone
Somalia
Sudan
Tanzania
Togo
Uganda
India
Indonesia
Malaysia
Pakistan
Iraq
Oman
United Arab Emirates
Yemen
Occupied Palestinian territories
Certain immigrant communities in:
– Australia
– Canada
– Europe
– United States of America
Prevalence of FGM in England and Wales
The prevalence of FGM in England and Wales is difficult to estimate because of the hidden nature of the crime. However, the Female Genital Mutilation (FGM) Enhanced Dataset (SCCI 2026) supports the Department of Health’s FGM Prevention Programme by presenting a national picture of the prevalence of FGM in England.
- There were 1,735 individual women and girls who had an attendance where FGM was identified in the period between April 2022 – June 2022. These accounted for 2,820 attendances reported at NHS trusts and GP practices where FGM was identified.
- There were 745 newly recorded women and girls in the period between April 2022 – June 2022. Newly recorded means this is the first time they have appeared in this dataset. It does not indicate how recently their FGM was undertaken, nor does it mean that this is the woman or girl’s first attendance for FGM. The number of newly recorded women and girls has reduced over time. This is to be expected as the longer the collection continues, the greater the chance of a women or girl having been recorded in it previously.
- Between April 2022 – June 2022, 78 NHS trusts and 17 GP practices submitted one or more FGM attendance records.
Source – https://digital.nhs.uk/data-and-information/publications/statistical/female-genital-mutilation/april-2022—june-2022
Consequences of FGM: Short & Long-term Implications, Mental Health & Wellbeing
FGM can cause a range of short-term and long-term health issues. The nature of the health implications arising from FGM are linked to the degree of the cutting, the cleanliness of the tools used to do the cutting, and the health of the person receiving the cutting.
In most countries, FGM is performed in unclean conditions by mainly traditional practitioners who may use scissors, razor blades, or knives. However, in some countries like Egypt, up to 90% of FGM is performed by a health care professional.
Short-Term Health Implications:
- Bleeding or haemorrhaging: If the bleeding is severe, the person can die.
- Infection: The wound can get infected and develop into an abscess (a collection of pus). A person can develop fevers, sepsis (a blood infection), shock, and may die if the infection is not treated.
- Pain: People are routinely cut without first being numbed or having anaesthesia. The most extreme pain tends to occur in the aftermath of the procedure.
- Trauma: People are held down during the procedure, which can be physically and psychologically traumatic.
Long-Term Health Implications (usually occurs to those with the most severe form of FGM):
- Problems passing urine. In severe cases, a person is left with only a small opening for urinating and menstrual bleeding. This can slow or strain the normal flow of urine, which can cause infections.
- Not being able to have sexual intercourse normally. The most severe form of FGM leaves a person with scars that cover most of their vagina. This makes sex very painful. These scars can also develop into bumps (cysts or abscesses) or thickened scars (keloids) that can be uncomfortable.
- Problems with gynaecological health. A person who has undergone FGM sometimes has painful menstruation. They may not be able to pass all of their menstrual blood. They may also have repeated infections. It can also be difficult for a health care professional to examine a person’s reproductive organs if they have had a more severe form of FGM. Normal tools cannot be used to perform a Pap test or a pelvic exam.
- Increased risk of cervical sexually transmitted infections (STIs), including HIV. People who have no medical training, under unclean conditions, perform most forms of FGM. Many times, one tool is used for several procedures without sterilisation. These conditions greatly increase the chance of spreading life-threatening infections such as hepatitis and HIV. Also, damage to the person’s sex organs during FGM can make the tissue more likely to tear during sex, which could also increase the risk of STIs or HIV.
- Problems getting pregnant, and problems during pregnancy and labour. Infertility rates among people who have undergone FGM are as high as 25 to 30% and are mostly related to problems with being able to achieve sexual intercourse. The scar that covers the vagina makes this very difficult. Once pregnant, a person can have drawn out labour, tears, heavy bleeding, and infection during delivery, which cause distress to the infant and the mother. Health care professionals who are unfamiliar with the scar will sometimes recommend a cesarean section. This is not necessary as an expectant mother will be able to deliver vaginally once the scar is cut open.
Mental Health & Wellbeing Implications:
FGM also affects mental health. Case histories and personal accounts from people note that FGM is an extremely traumatic experience that stays with them for the rest of their lives.
Research carried out in Dakar, Senegal (see FGM Trauma.pdf (taskforcefgm.de))confirmed that people who had undergone FGM showed an appreciably higher occurrence of Post-Traumatic Stress Disorder (PTSD) (30.4%) and other psychiatric symptoms (47.9%) than those who had not undergone the procedure.
Practitioners should be aware of the potential manifestations of psychological dysfunction in victims of FGM. Whilst many people presenting for counselling who have been victims of childhood abuse display symptoms of PTSD, this diagnosis is not the only psychological difficulty that victims may encounter. They also include:
- FGM may be a contributory factor to psychological distress
- Presenting the issue may be something different
- Feelings of ‘nothingness/incompleteness/ anxiety/low self-esteem
- Lack of trust
- Anger or depression resulting from the suppression of anger
- Fear of marriage and sexual relationships
- Fear of childbirth
- Loss
- Fear for their daughters
- Denial of sexuality and focus on reproductive functions
- Flashbacks
- Lack of sexual responsiveness
The above is not an exhaustive list,
Links to forced marriage and honour-based violence
A forced marriage is where one or both people do not (or in cases of people with learning disabilities or reduced capacity, cannot) consent to the marriage as they are pressurised, or abuse is used, to force them to do so. It is recognised in the UK as a form of domestic or child abuse and a serious abuse of human rights.
The pressure put on people to marry against their will can be physical (including threats of intimidation, actual physical violence and sexual violence) or emotional and psychological (for example, when someone is made to feel like they’re bringing shame on their family). Financial abuse can also be a factor.
For more information, visit:
- https://www.gov.uk/forced-marriage
- https://www.gov.uk/government/uploads/system/uploads/attachment_data/file/322310/HMG_Statutory_Guidance_publication_180614_Final.pdf
In certain communities, it is considered important that a person undergo FGM before being able to marry. Usually, this will be performed during childhood, but nationally, there have been reports of people undergoing FGM just before a forced marriage.
‘Honour’ based violence (HBV) occurs when perpetrators believe a relative or other individual has shamed or damaged a family’s or community’s ‘honour’ or reputation (known in some communities as izzat), and that the only way to redeem the damaged ‘honour’ is to punish the individual, which may result in severe injury or death. HBV is a term that is widely used to describe this sort of abuse; however, it is often referred to as ‘honour’ based violence because the concept of ‘honour’ is used by perpetrators to make excuses for their abuse.
There is a strong link between ‘honour’ based violence, forced marriage and domestic abuse (please also see the NYSCP Domestic Abuse Practice Guidance or the CYSCP Domestic Abuse webpage). Examples of ‘damaged honour’ are:
- Defying parental authority
- Becoming overly westernised in style (e.g. clothing, make-up, behaviour, attitudes, etc.)
- Having sex/relationships/pregnancies outside marriage
- Using drugs, alcohol, and cigarettes
- Family honour can be damaged by unfounded or untrue gossip or rumours
- Interfaith or intercommunity relationships
- Leaving a spouse or seeking a divorce
In order to control the actions of children, young people and adults, either to prevent a person from bringing shame to a family or community, or punish them for doing so, FGM may be used.
Other forms of ‘honour’ based violence can include, but are not limited to:
- Being disowned or ostracised by the community
- Physical abuse of the victim by family members, including spouse and in-laws NYSCP Domestic Abuse Practice Guidance or CYSCP Domestic Abuse webpage
- Restriction of freedom or loss of independence – being “policed” by family members
- Isolation from wider family or community, e.g. stopped from seeing friends
- Forced marriage
- Murder
Internalisation of guilt or shame by the victim can cause internal conflict for them, and not wanting to cause further shame can result in self-harm and suicide attempts.
Requests for Female Genital Mutilation medical examination in under 18-year-olds in the emergency department
Female genital mutilation (FGM) is defined by WHOas procedures which removes or damages the external female genital organs for no medical reason. It is illegal in the UK and regulated teachers, health and social care staff have a mandatoryreporting duty to inform the police when:
- a girl disclosing that she has been subjected to FGM or
- physical signs are observed which appear to show that an act of FGM has been carried out on her.
In some cases, this may lead to a medical assessment being requested. Variance exists across England about how and where girls under the age of 18, who may have been subjected to FGM, receive medical examinations.
Confusion in the system from a concern being raised through to examination has led to examples of girls being examined multiple times due to lack of expertise in the examiner to diagnose and/ or lack of appropriate recording via colposcope of the examination to enable second opinion. This can have a significant impact on the girl and her family causing additional stress and trauma to an already difficult circumstance.
In some instances, girls are accompanied to the emergency department by social services and/or police who request an examination of the girl to determine if FGM has occurred. The clinician may feel pressure to agree if there is a risk the girl is separated from family until a diagnosis is given.
However, unless there is concern about an acute injury requiring urgent medical intervention (in which case, clinicians should follow their normal protocol and safeguarding procedures), clinicians should decline the request to examine for the purpose of FGM diagnosis or opinion. They should inform the Trust safeguarding lead of the request so appropriate follow up and escalation can occur with the wider system.
FGM diagnosis, particularly in children, is a highly specialised skill.
It is accepted that it would be inappropriate for a child to be bought to the emergency department solely for a child sexual abuse examination. The same approach must be adopted for FGM.
Skills and location required for paediatric FGM examination
The Royal College of Paediatric and Child Health (RCPCH)’s safeguarding roles and competencies for paediatricians states that paediatricians undertaking assessments of children who may have experienced FGM need to be trained and competent.
The Department of Health and NHS Service standards for FGM highlights that in all cases involving children, an experienced clinician should be involved in setting up a sensitive, thorough paediatric examination that allows for the maximum opportunity to confirm diagnosis of FGM and related injuries, agree a treatment or support plan and aid criminal investigation.
Clinics/services offering confirmation of FGM should include: • Paediatrician with experience of examining children’s genitalia, using colposcopy and writing legal reports.
- Clinicians with good knowledge of the types of FGM and the physical symptoms and signs as they present in under 18s.
- Protected time for the preparation of statements and reports for child protection enquiries, criminal investigations and the courts; have protected time for court attendance; and undergo case supervision and regular peer review.
- Sufficient throughput of cases; clinicians must have experience of examining enough cases of child sexual abuse and/or FGM to maintain skills and competency as recommended by the Royal College of Paediatrics and Child Health.
Safeguarding
Although the emergency department is not the appropriate setting to determine whether a girl has been subjected to FGM, if a girl is brought for an FGM examination normal safeguarding procedures should still be followed to determine if other safeguarding concerns are present.
Appropriate Examination Process
As per the Government Working together to safeguard children, a strategy meeting should be held between the statutory partners (Health, Social Care and Police), to determine the child’s welfare and plan rapid future action if there is reasonable cause to suspect the child is suffering or is likely to suffer significant harm. The role of the (appropriately skilled and experienced), health practitioner is to advise about the appropriateness or otherwise of medical assessments. The appropriate time and location of any medical assessment should be agreed upon at the meeting.
Useful numbers
Afruca-Africans Unite Against Child Abuse
Unit 3D/F, Leroy House,
436 Essex Road
London, N1 3QP
Tel: 0207 704 2261
Email: info@afruka.org
Website: www.afruka.org
Black Health Initiative (BHI)
231 Chapeltown Road
Leeds LS7 3DX
Tel: 0113 3070300
Website: www.blackhealthinitiative.org
Black Women’s Health & Family Support
First Floor
82 Russia Lane
London
E2 9LU
Tel: 020 8980 3503
Email: bwhafs@btconnect.com
Website: http://www.bwhafs.com
Childline
Tel: 0800 1111
Website: www.childline.org.uk
FORWARD- Foundation for Women’s Health Research and Development
Suite 2.1
Chandelier Building
8 Scrubs Lane
London
NW10 6RB
Tel: 020 8960 4000
E-mail: forward@forwarduk.org.uk
Website: www.forwarduk.org.uk
Halo Project
The Halo Project, an award-winning specialist service provider supporting Black, Asian and Minority Ethnic (BAME) victims and survivors of illegal cultural harms, such as forced marriage, female genital mutilation and honour-based abuse, has partnered with Yorkshire’s largest domestic abuse and sexual violence charity, IDAS, to intensify the level of support offered to victims and survivors across the region.
For more information, visit:
Home Office FGM Unit
Tel: 0800 028 3550
Email: fgmenquiries@homeoffice.gsi.gov.uk
Website: www.gov.uk/government/collections/female-genital-mutilation
IDAS
IDAS is the largest specialist charity in Yorkshire supporting people affected by domestic abuse and sexual violence.
NSPCC FGM Helpline
Tel: 0800 028 3550 (24-hour free helpline)
Email: fgmhelp@nspcc.org.uk
Website: www.NSPCC.org.uk
References and Further Reading
WHO Female Genital Cutting Key Fact Sheet
https://www.who.int/news-room/fact-sheets/detail/female-genital-mutilation
Eliminating Female genital mutilation, World Health Organisation
FGM Key Facts, World Health Organisation
http://www.who.int/mediacentre/factsheets/fs241/en/
Female Genital Mutilation – The Facts, HMG
https://www.gov.uk/government/publications/female-genital-mutilation-leaflet
Page reviewed: March 2026




 View all our news
View all our news